Lumbar Spinal Stenosis
Minimally invasive surgery for Lumbar Spinal Stenonis
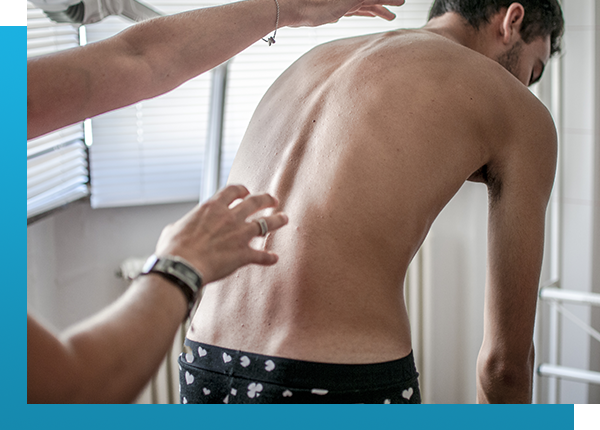
Spinal Stenosis
Spinal stenosis is a condition that is quite common. It results in narrowing of the spinal canal either in the cervical, thoracic or lumbar region. If spinal stenosis is symptomatic, it will require treatment. Patients may have MRI/CT scans that indicate spinal stenosis, but if they are asymptomatic, there is no need for treatment.
Lumbar spinal stenosis is the most common. It is present as central, recess and/or foraminal stenosis. Symptoms may all be the same. But when recess and foraminal stenosis is also present, radicular (sciatica-like) symptoms may also be present.
If you or a loved one is living with this condition, then you may want to read further to learn about the diagnosis and the procedures and treatments available. Contact the Center for Pain Management in New Jersey if you are interested in proceeding with any of our treatment options or if you would like some more information about Lumbar Spinal Stenosis. Our trusted team is here to help educate you on this spinal condition and answer any questions you may have.
Lumbar Spinal Stenosis (LSS)
LSS is a painful condition and the incidence is about 1.1 million patients. It is expected to rise with the aging population. In addition, it is the commonest indication for spinal surgery in the elderly. In the normal anatomy of the vertebra, discs act as shock absorbers, protect the spinal cord and create space for the nerves to exit. Flexion or bending forward will open the spine and extension or bending backwards will close the canal.
In a stenotic spine, with age, the canal gets narrow, causing pressure on nerves, resulting in pain, numbness and tingling. Pain may extend from the back to the buttocks and legs. Symptoms are most notable when standing. This results in difficulty with doing daily chores including brushing your teeth, shaving, standing to shower. Leaning or bending forward results in the opening of the spinal canal and reduction of pressure. This is why we see so many older patients walking in shopping malls with a cart. They are able to lean in front and relieve pressure. Sitting will also have the same effect. Patients who sleep on their backs may wake up with pain as their spine is extended.
Presentation may also include issues with balance, and a decreased endurance for physical activity. Significant decrease in ability to walk any length. To confirm neurogenic claudication, 2 simple steps need to be taken. If patients are symptomatic with standing, with numbness, and feel better with bending, or sitting, claudication is the most likely cause. Spinal stenosis is a burden for the patient and society. As a result of decreased activity, obesity is very common, decrease in physical endurance, psychological issues, including depression, and deterioration of other medical comorbidities. Spinal stenosis is diagnosed using a combination of signs and symptoms and radiological investigations. MRI is the preferred choice, but in some cases, CT scan is the only choice.

Treatments
Treatment of spinal stenosis must always start with conservative measures. These include physical therapy, weight management, non-steroidal medications etc. If necessary various pain interventions may be tried. It is good to remember that in the presence of spinal stenosis, which is probably partially caused by facet hypertrophy(spondylosis), lumbar medial branch nerve block may be indicated and helpful. Epidural injections may be helpful, but there are limits on the number of interventions that can be offered. These injections do help to reduce inflammation, but may stop being effective.
It is always recommended to seek out consultation with a spine surgeon regarding options for surgery. Surgical options include laminectomy, laminectomy with fusions, microdiscectomy, etc. Surgery may not be an option for all patients because of various reasons. These include patient reluctance, patient health issues, patient desire to try less aggressive options before major spine surgery. These situations are best served by Minimally Invasive Surgery for Lumbar Spinal Stenosis.
There are two options available for patients. One is Minimally Invasive lumbar decompression (MILD) and the other is Indirect Lumbar Decompression (Vertiflex). MILD and Vertiflex are both outpatient procedures performed by highly trained pain management physicians. The procedures can only be offered to patients with lumbar spinal stenosis. MILD can be done from L1-2 to L5-S1. Vertiflex can be done from L1-2 to L4-5.
MILD is done by removing excess tissue in the epidural space using a 5.1 mm incision on both sides. Specially designed instruments are used. Most often it is necessary to address one level. Occasionally there is a need to address two levels. This can be done via the same incision. There are no stitches at the end, and patients go home the same day.
Vertiflex is also an outpatient procedure that is done via a midline incision about 1 cm long. In this procedure we are able to place a stent like device that keeps the spine open and reduces the pressure on the nerves. This is done with specially designed instruments. There is a need to close the small incision with sutures. All patients go home the same day. Usually one space is addressed, but occasionally we need to do two levels. This is through the same incision.
Results from these procedures may vary, but response rate has been about 80-85%. There have been no serious complications noted. All patients will need to do physical therapy after the procedure. Vertiflex patients need to be careful about bending after the procedure and start physical therapy about 6 weeks after the procedure. It is extremely important to remember that after MILD or Vertiflex procedures, there is no contraindication for major spinal surgery as these procedures do not change spinal anatomy.
After reading about spinal stenosis and lumbar spinal stenosis, you may have many questions. Whether your questions are related to the signs, symptoms and diagnosis of this condition or our treatment options, we are here to give you the answers you seek. As we have noted earlier, the results from these treatments and procedures may vary, depending on the severity of your condition and your body. Our experienced team has the insight to advise you on which treatment or procedure will suit you the best. You can learn even more about what the Center for Pain Management in New Jersey has to offer, in terms of knowledge and advice, by contacting our staff today. Let our trusted team guide you through this process.
